PADICE Surgical Implant Program
Sessions 7–9: Advanced Bone, Soft Tissue & Esthetic Implant Surgery
INTRODUCTION
Sessions 7, 8, and 9 represent the advanced regenerative and esthetic phase of the PADICE Surgical Implant Program. These sessions are designed to train clinicians in the biological reconstruction of deficient alveolar ridges and the esthetic placement of implants in high-risk zones, particularly the anterior maxilla.
The focus of Sessions 7–9 is on bone augmentation, soft-tissue management, membrane-based regeneration, PRF-assisted healing, and esthetic implant placement. Participants learn to treat patients with horizontal and vertical bone deficiencies, thin biotypes, and compromised esthetic zones using modern regenerative and microsurgical principles.
These sessions form the bridge between routine implant placement and advanced implant reconstruction, allowing clinicians to treat complex grafting and esthetic cases with predictability and safety.
PRIMARY CLINICAL FOCUS
- Guided bone regeneration (GBR)
- PRF-based regenerative dentistry
- Piezosurgery for bone harvesting and site development
- Particulate and block bone grafting
- Membrane-based ridge augmentation
- Soft-tissue augmentation around implants
- Esthetic anterior implant placement
- Management of grafting complications
- Anterior single-tooth implant placement
COURSE OBJECTIVES
Upon completion of Sessions 7–9, participants will be able to:
Foundations of Regenerative Implant Dentistry
Recognize the biological principles of bone and soft-tissue regeneration
Understand the indications for grafting in implant dentistry
Define the goals of ridge augmentation for functional and esthetic implant placement
Bone Grafting & Regenerative Biology
Understand the biology of bone healing and graft incorporation
Apply the principles of osteoconduction, osteoinduction, and osteogenesis
Use PRF to enhance wound healing and bone regeneration
Diagnostics, Imaging & Surgical Planning
Interpret CBCT imaging for ridge defects and graft planning
Plan staged versus simultaneous GBR procedures
Identify anatomical limitations and risk zones for grafting and anterior implants
Treatment Planning for Compromised Sites
Formulate treatment plans for bone-deficient ridges
Select appropriate grafting approaches:
- Particulate grafting
- Block grafting
- Membrane-based GBR
Design treatment plans for esthetic anterior implant placement
Surgical & Clinical Competence
Perform particulate bone harvesting and graft placement
Perform membrane-based GBR
Perform block grafting procedures
Execute anterior single-tooth implant placement
Perform incision line opening and flap management for regenerative surgery
Manage soft-tissue augmentation around implants
Esthetics & Soft-Tissue Management
Design implant placement for esthetic outcomes
Augment peri-implant soft tissue using grafting materials
Control tissue contours for anterior implant restorations
Complication Prevention & Management
Recognize and manage bone grafting complications
Identify early signs of graft failure or soft-tissue breakdown
Implement corrective strategies for compromised regenerative cases
CORE TOPICS
- Keys to successful bone grafting
- PRF in regenerative dentistry
- Piezosurgery in implant dentistry
- Particulate bone harvesting techniques
- Membrane grafting
- Staged vs simultaneous GBR
- Anterior single-tooth implant placement
- Esthetics and anterior implant placement
- Soft-tissue augmentation techniques and materials
- Bone grafting complications
- Incision line opening
HANDS-ON TRAINING
Participants will complete the following laboratories and live surgical training:
- CT-based treatment planning
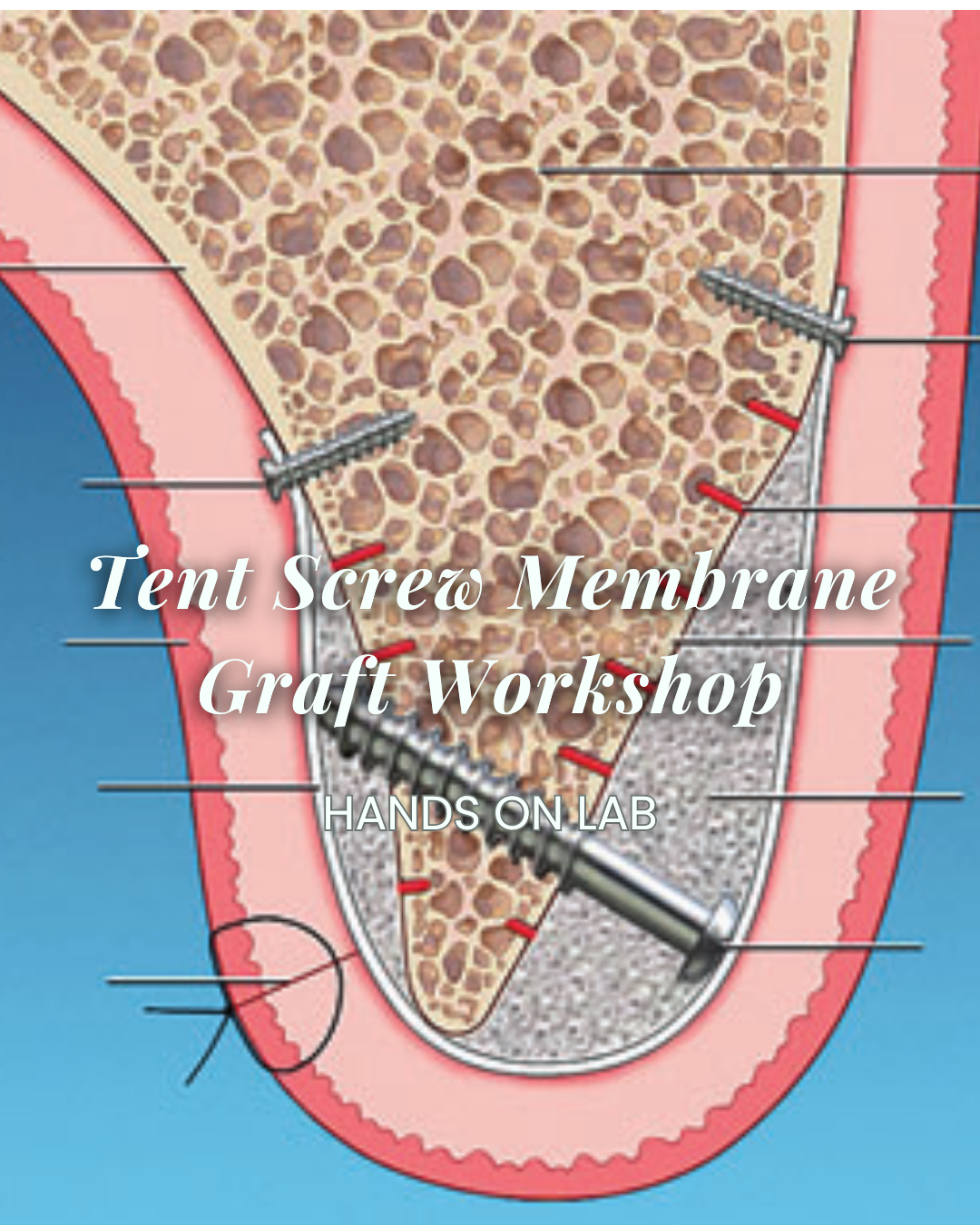
- Tent screw membrane graft workshop
- Ramus harvest laboratory workshop
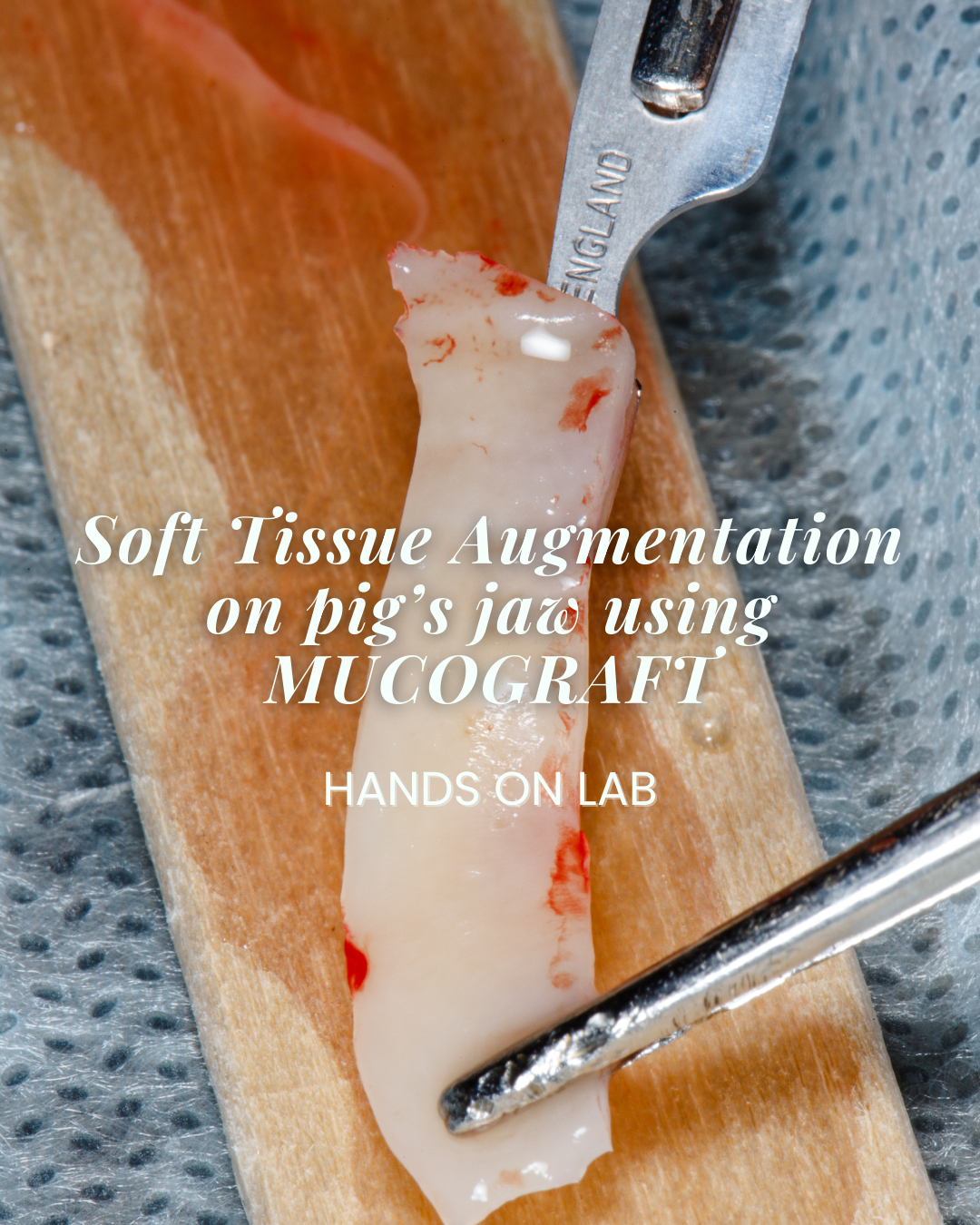
- Soft-tissue augmentation on pig’s jaw using Mucograft
- Onlay block grafting workshop
- Live surgery